Julien Riou writes:
Stan epidemiologist here. We actually just released a preprint [estimating death rates of people infected with coronavirus, breaking down the population by age and then poststratifying] using Stan (https://www.medrxiv.org/content/10.1101/2020.03.04.20031104v1).
Crude estimates of case fatality ratio obtained by dividing observed deaths by observed cases are biased in two ways:
1) Deaths are underestimated because of the delay between disease onset and death (right censoring);
2) Total cases are underestimated because surveillance efforts focus on severe cases and miss asymptomatic and mild cases.
We attempted to correct for both these biases using data from China and a few assumptions. It might still need some refinement though, happy to hear any comment.
And here’s the paper by Julien Rieu, Anthony Hauser, Michel Counotte, and Christian Althaus:
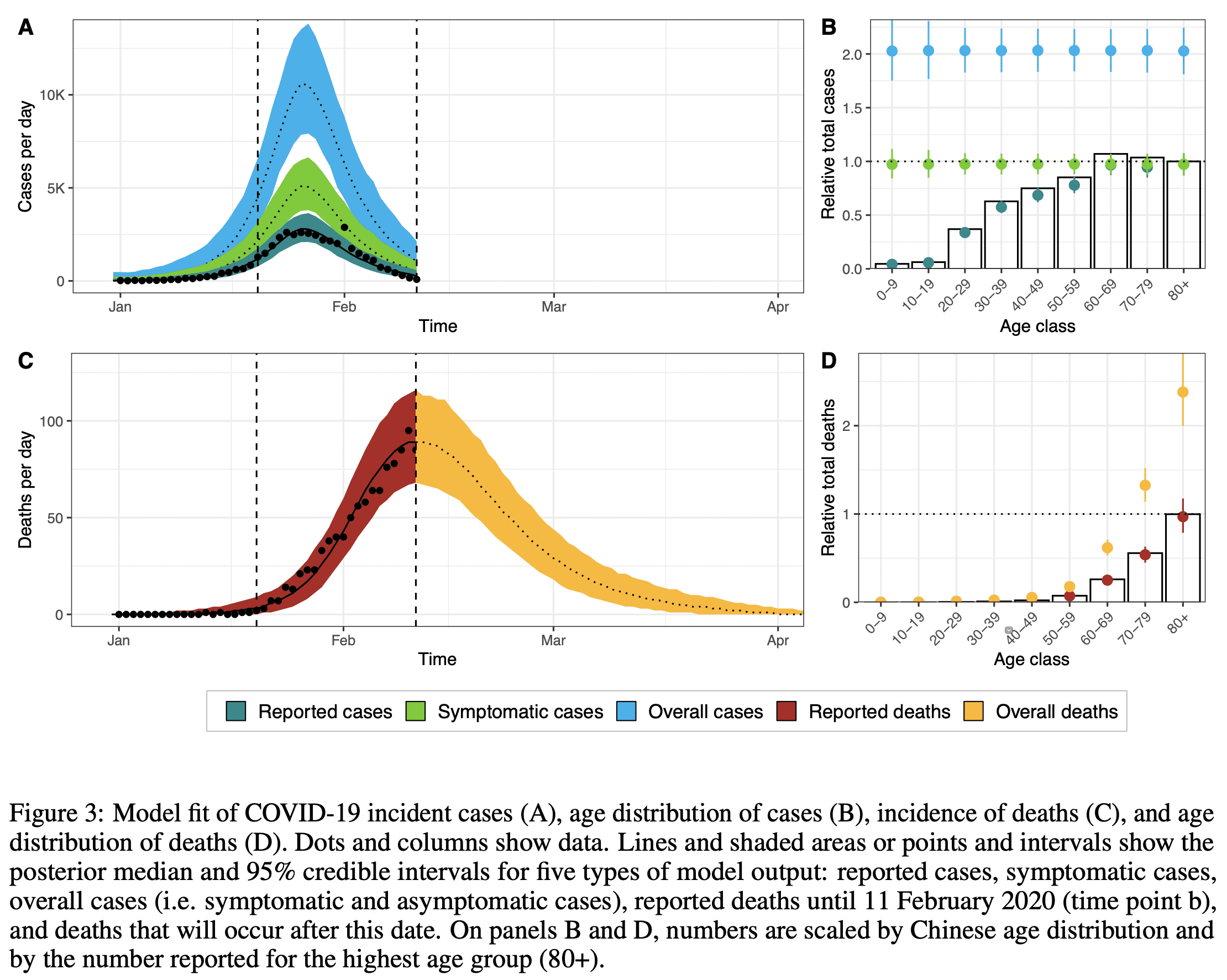
We [Riou et al.] estimated the age-specific case fatality ratio (CFR) by fitting a transmission model to data from China, accounting for underreporting of cases and the time delay to death. . . . We find that 1.6% (1.4-1.8) of individuals infected with COVID-19 [in Hubei between 1 Jan and 11 Feb] with or without symptoms died or will die, with even more important differences by age group than suggested by the raw data. The probability of death among infected individuals with symptoms is estimated at 3.3% (2.9-3.8), with a steep increase over 60 years old to reach 36% over 80 years old.
The narrowness of these intervals implies that these are inferential uncertainties conditional on the model and do not account for uncertainty in the model itself.
Here are some more graphs from the paper:
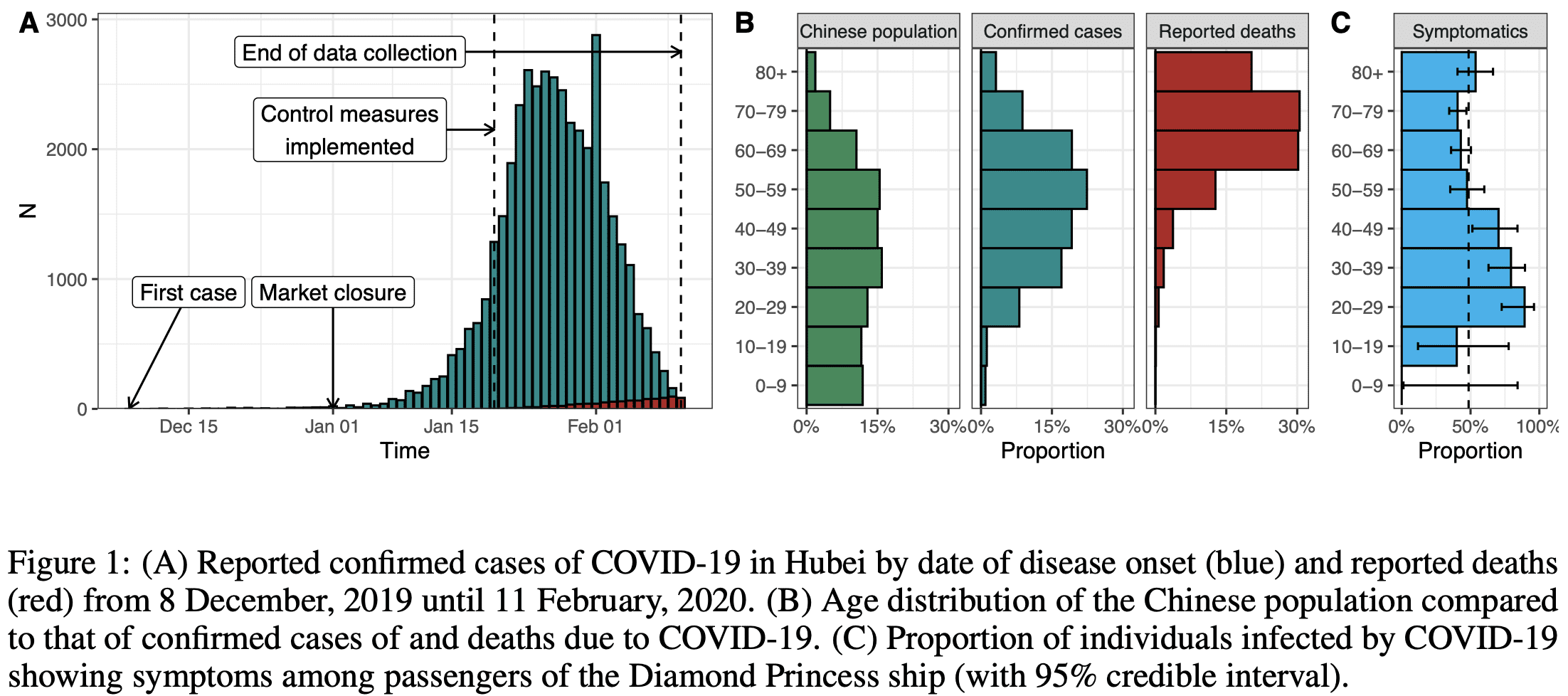
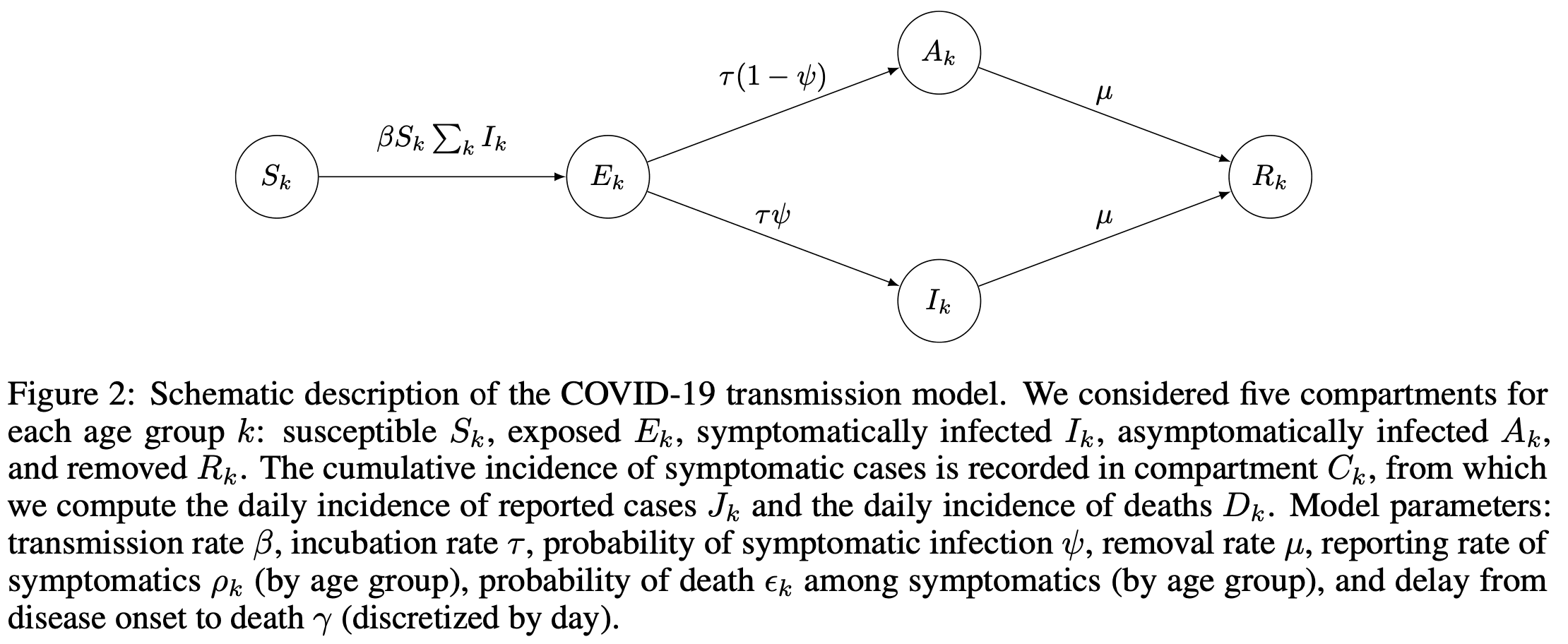
Strengths of the analysis
Here’s how Rieu et al. describe the strengths of their work:
(1) We use a mechanistic model for the transmission of and the mortality associated with COVID-19 that is a direct translation of the data-generating mechanisms leading to the biased observations of the number of deaths (because of right-censoring) and of cases (because of surveillance bias). Our model also accounts for the effect of control measures on disease transmission. (2) Our model is stratified by age group, which has been shown as a crucial feature for modelling emerging respiratory infections [16]. (3) The estimates rely on routinely collected surveillance data such as incident cases by disease onset, incidence deaths, and the age distribution of cases and deaths, and does not require individual-level data nor studies in the general population.
Limitations
The paper continues with a list of limitations:
(1) Our results depend on the central assumption that the cause of the deficit of reported cases among younger age groups is a surveillance bias and does not reflect a lower risk of infection in younger individuals. The reason for this age shift is unknown [10]. Retrospective testing for COVID-19 of samples from influenza-like-illness surveillance found no positive test among children, but the sample sizes were small (20 per week including both adults and children) [10]. Uneven age distributions in the risk of infection can be attributed to immunological features, such as the lower circulation of H1N1 influenza in older individuals due to residual immunity [17]. An immunological explanation of the opposite phenomenon, with a lower susceptibility of younger individuals, seems unlikely, and there is no indication of pre-existing immunity to COVID-19 in humans [10]. Different contact patterns could play a role in a limited outbreak, but not in such a widespread infection, especially as household transmission seems to play a major role [10]. The last explanation that we assume here is that younger individuals, when symptomatic, have milder symptoms that decrease the probability of seeking care and being identified.
(2) In a related matter, our results depend on the assumption that older individuals have more severe symptoms and are more likely to be identified. In the absence of an outside reference point, the reporting rate cannot be estimated from surveillance data only. We chose to fix to 100% the reporting rate of infected individuals that have symptoms and are aged 80 and more, and estimate the reporting rates in other age groups relatively to that of older individuals. If further data, coming from a study in the general population, shows that this assumption is violated, this would lead to an overestimation of the CFR in our study.
(3) There is important uncertainty around the proportion of asymptomatic infections. Currently, the detection of asymptomatic patients in China is limited by the focus on symptomatic patients seeking care and the lack of seroprevalence data [18]. The proportion of symptomatic infections has been estimated to 58% (95% confidence interval: 33-83) in a small sample of cases exported to Japan [19]. During the outbreak on the ship “Diamond Princess”, nearly all individuals were tested regardless of symptoms, leading to an average proportion of symptomatic infections of 49% in a sample size of 619, which was used in the present study [13]. Still, uncertainty about the proportion of symptomatic infections will remain until a large retrospective seroprevalence study is conducted in the general population, and our results are dependent on this estimate. Additionally, the dichotomization of infection into asymptomatic and symptomatic is a simplification of reality; the infection with SARS-CoV-2, will likely cause a gradient of symptoms in different individuals depending on age, sex and comorbidities [10]. The proportion of asymptomatic infections might show an age-dependent structure.
(4) Our findings regarding the CFR are specific to the context, and should be interpreted in that light. The findings describe the situation in Hubei from 1 January to 11 February, 2020. It was demonstrated there, that mortality rates have changed over time as a result of an improvement of the standard of care [10]. The standard of care and, as a result, the CFR is setting-dependent and cannot be directly applied to other contexts.
I have not read this paper carefully or tried to evaluate their model or their claims.
P.S. Riou adds:
All data and code is available on https://github.com/jriou/covid_adjusted_cfr, the stan code is in model/model10.stan and the data is obtained and formatted in run_models.R. The model is computationally intensive, about 1 day on our cluster here in Switzerland.
The idea of the model is some kind of post-stratification, backed by an epidemic SIR-type model implemented in ODEs. I made some improvement on model10, including another source for the proportion of symptomatics (and using a distribution not a fixed proportion), and adding data about the contacts between age groups in China. It’s still running, I will upload it to github now (model11 and model12).
P.P.S. Someone pointed me to another paper that uses a differential equation analysis, “Substantial undocumented infection facilitates the rapid dissemination of novel coronavirus,” by Ruiyun Li, Sen Pei, Bin Chen, Yimeng Song, Tao Zhang, Wan Yang, and Jeffrey Shaman. I haven’t read this one carefully either. Data and code are here, and this is their summary:
Estimation of the prevalence and contagiousness of undocumented novel coronavirus (SARS-CoV2) infections is critical for understanding the overall prevalence and pandemic potential of this disease. Here we use observations of reported infection within China, in conjunction with mobility data, a networked dynamic metapopulation model and Bayesian inference, to infer critical epidemiological characteristics associated with SARS-CoV2, including the fraction of undocumented infections and their contagiousness. We estimate 86% of all infections were undocumented (95% CI: [82%-90%]) prior to January 23, 2020 travel restrictions. Per person, these undocumented infections were 55% as contagious as documented infections ([46%-62%]) and were the source of infection for two-thirds of documented cases. These findings explain the rapid geographic spread of SARS-CoV2 and indicate containment of this virus will be particularly challenging.
Jeff Shaman, one of the authors of that paper, writes:
I find it hard to believe that 1.6% of all infections died—the case fatality rate in China was 2.38% as of February 11th, the majority of that driven by activity in Hubei. The rapid spread of the virus geographically, serological evidence from evacuees, and our own work, indicate that only 10-20% of infections were confirmed cases. The CFR is deaths/confirmed cases. If one-tenth to one-fifth of infections are confirmed cases that implies 0.238% – 0.476% of all infections died.
P.P.P.S. More here.
I don’t think Hubei is going to be a good example, I’ve posted this before: https://www.youtube.com/watch?v=Kd4YNiPcjdw
I also see all modellers are still ignoring that people are effectively spreading this thing on purpose in all the countries with a lot of cases. In China they were spitting on healthcare workers, rubbing used tissue on elevator buttons, etc. In South Korea most cases are from a Church with mandatory attendance and very close contact during prayer. In Italy the government was putting out public service announcements in early Feb telling people to hug Chinese tourists. In Iran people are licking a shrine to get the virus.
Hubei was overwhelmed by cases due to fast transmission followed by a rapid peak in cases. They did whatever they could to isolate people as much as possible. they should have done better but obviously were working under very adverse conditions.
I’ve been saying for a while, early isolation is the only thing that will avoid such fast peak plus overwhelming outside China. if we let this thing spread we will need these kinds of field quarantines and have many deaths… the alternative is widespread social distancing starting NOW which will dramatically slow the growth in case numbers and lead to hospitals being able to treat… there’s no other good choices available at the moment.
Sorry, reply showed up below (browser reloaded the tab or something).
Early isolation is fine. But how do you do early identification?!
I mean isolation of healthy people from each other. work from home, close schools and universities, cancel conferences, don’t go to gyms, pools, church, AA meetings, libraries elderly people should get grocery deliveries, etc etc
Is it clear that the economic downside of such drastic isolation measures aren’t worse than tolerating a baseline infection rate, mitigated by whatever less drastic measures (washing hands, isolating symptomatic cases, ) may be taken?
I think so, I mean I’ve only done back of envelope. But let’s put it this way, I offer you the following deal: I will deposit $X into an account for your heirs. After you confirm the dollar transfer you will take a cyanide pill and die.
What $X will you be willing to accept this? You can also ask the question, at what dollar amount would an insurance company be willing to insure your life without fear that you will simply commit suicide to get the money for your family?
I put the number well above $10M for me given that I have two children who are already reasonably economically secure etc. I certainly wouldn’t commit suicide if I had a $10M insurance policy.
Now, I’m mid 40’s so my risk of death is on the order of 0.005 from getting this disease. 0.005 x $10M = $50k which is more or less same range as GDP/capita. So at least people like me should be willing to stop all economic activity for on the order of a year.
Obviously, we need food, and healthcare and etc.
The next thing we need to realize is that economic activity delayed is not economic activity LOST. If I was planning to remodel my bathroom and I wait until after COVID, and do it next October instead… well the loss is just the cost of moving those dollars out 7 months… at current interest rates this is basically zero.
Now, for people over 60, the risks go up A LOT but the willingness to accept death dollar amount might go down. Obviously if you’re 98 and have family you care about, you might well be willing to accept $10M to your grandchildren in order to take a cyanide pill.. but the end result is not going to change by 2 orders of magnitude or anything.
But whether you fiddle these numbers around one way or another the unavoidable conclusion is except for life-sustaining activity, we should all be willing to stop at least 50-80% of all economic activity over a period of at least a couple to three months in order to avoid something even in the order of magnitude of this severe.
> The next thing we need to realize is that economic activity delayed is not economic activity LOST.
You have to be a little more careful with that statement. There is probably some slack, but also some loss. If everyone postpones, then for the next six months the carpenter won’t be working for six months. So when you go decide to remodel, and someone else does as well, whereas he before could have remodeled both, he now has to pick one or the other. For the carpenter, this means less output. For the economy, this means less value created (someone will have to suffer with their old kitchen for longer than they had planned).
True enough but this delayed gratification is precisely what the discount rate measures. You can argue that at the moment the “real” discount rate and the current govt manipulated one are not the same… but if you are willing to go with the market rates, they are extremely low, so a benefit a year out is only a percent or two or three less value than the benefit today.
Daniel, when you say “economic activity delayed is not economic activity LOST” it sounds as if you mean that what is not done now will be done later in addition to what would have been done later anyway. This may be true in some sectors but is less true in others. If one unit of kitchen remodelling is delayed forever it’s effectively lost.
(Or maybe you were conceding the point, I’m not sure what the discussion about discount rates in your reply to Simon was about.)
Carlos, the naive way to look at someone doesn’t remodel their bathroom this month is that this is say $10,000 lost.
The proper calculation is that this $10,000 project is delayed say six months, which at say 3% interest rate means it’s now worth exp(-.03*0.5)*10000 ~ 9851 today so around $150 lost on this project… in general you could say that the value of everything to be done in the future all dropped by 1.5%. If you buy into the idea that there is negative interest rates on some loans… the value actually increased instead!
IMHO the biggest problem here is govt manipulated interest rates don’t reflect actual preferences. its like price fixing on gasoline distorts economic activity or whatever
Daniel
Your analysis doesn’t make sense. You could plug in the risk for almost any everyday activity ending up deadly. Ultimately you would have to take the pill and collect the 10M.
Johannes,
Everyday risks are already priced in to the equation. If I told you you could take the pill and get the $10M or you could live in solitary confinement eating a minimal diet not exercising and not free to leave… you’d probably take the pill.
Risks and benefits of your everyday life balance out evidently and it’s worth it to you to drive around and go hang gliding because this is the reason you are living.
when you add a marginal risk that has no inherent benefit (I don’t know many people who enjoy being sick, lots of people enjoy hang gliding or parachuting or whatever) it’s a different story.
Given how much of what people do these days is bullshit, it might well be BETTER economic outcomes if half of all office workers went home and then never came back… :~)
Very true, I’ve often said I’d rather take the NIH grant money and pay people to stay home instead of produce their NHST-based misinformation and obstacles. The same is probably true in many other cases.
There’s a whole Reddit group …
https://www.reddit.com/r/BullshitJobs/comments/f9q77m/im_a_professional_copypaste_worker_making_over/
Daniel:
That reminds me . . . recently I’ve been doing something for a consulting project where I need some data. I keep sending emails and filling out text boxes to try to contact the vender. Every once in awhile I receive a reply, each time it’s from a different person, it’s never what I need. It’s almost like they are trying to avoid making money on this one!
The reason early isolation is important if not critical is that it provides time to identify how the pathogen transmits and time to develop vaccines. It may also reduce the virulence. The sooner isolation is imposed the more likely it is to be effective.
Last but not least if you wait to long the economic impact could be much greater.
I’m surprised that this is such controversial idea. A few weeks of economic slow down now is better than a month or more of total shutdown as in Wuhan.
Early was 2 months ago, and I doubt there will be a safe vaccine since there never was for SARS.
there was no need for sars it hit on the order of 1k people and was squashed by isolation interventions
It’s research so no one will know when, but expanded research efforts have been ongoing in many places for some time e.g https://cihr-irsc.gc.ca/e/51868.html
I did hear an educated guess of 3 months back in January. Again no one knows for sure.
Well, they managed it in Wuhan. Days from illness onset to diagnosis was reduced from an average of 15-28 days to 4 days.
Countries should follow Singapore’s lead! In Singapore, we’ve been able to lead relatively normal lives during the past 6+ weeks the disease has been with us, but:
(1) Anyone who has been in a high-risk area (northern Italy, South Korea, China, Iran) has to self-isolate for two weeks, regardless of whether they are symptomatic.
(2) Anyone who has respiratory symptoms stays home from work/school regardless of whether they have been in contact with a known COVID-19 case.
(3) Large events are mostly canceled.
(4) People are much more careful with washing their hands than usual (you really can tell the difference in public bathrooms).
These measures (along with intense contact tracing and swift isolation) seem to have been very effective at containing the disease, at least for now, and they’re much less extreme than what’s been done in China.
Singapore has half the population of LA county and is isolated by being an island. it has many advantages compared with most of the world when it comes to viral pandemics.
It also has many disadvantages: it’s very densely populated; most people live in large apartment buildings; most people eat out in large food courts rather than cook at home; most people don’t have their own car but depend on public transportation; and it’s a major airport hub connecting together Asia, Australia, America, and Europe.
This sounds reasonable. You really think large events are more of a danger than eg public transportation though? I’d say another protective measure should be that people drive to work in their own cars if possible.
Probably not, but very few people in Singapore have a car.
Plus, Singapore has temperatures around 30 degrees Celsius which should hamper the virus significantly. I think that factor alone might eclipse all the others.
Life in Singapore mostly takes place indoors, in air conditioning, so I doubt the temperature plays a significant role. Singapore even has a flu season, which can be just as severe as in the rest of the world.
AC in a hot, humid environment can be a positive for mitigating viral spread because it raises relative humidity. Helps minimize aerosols from coughs, sneezes, etc. I believe humidity that is too high does become counterproductive, however.
Air conditioning reduces indoor humidity.
Olav: Thanks for providing a view from Singapore.
Olav:
I agree. Singapore seems to have struck the right balance between epidemic control versus economic disruption.
Lot more reasonable than some of the other, more radical prescriptions I am reading being advocated.
It is not a coincidence that China, South Korea and Italy are all conducting lots of tests. The amount of testing done has got to be in any model.
I am so sorry that your listed facts about China/Italy were true but rather biased. F words here.
But you are fine with bias against people licking a shrine in Iran?
The US has it’s own spreaders, like the touchscreen robot in Times square that encourages sick people to touch it and tells you if you have the symptoms: https://nypost.com/2020/02/11/creepy-coronavirus-screening-robot-returns-to-times-square/
Or these people: https://www.denverpost.com/2020/03/03/candi-cdebaca-tweet-coronavirus-maga-rallies/
So don’t worry, there will be many cases in the US.
I would have loved to see the script (code) of the estimated model in Riou et al.
At first glance I didn’t see it, but here it is:
https://github.com/jriou/covid_adjusted_cfr
Yes the code in on
https://github.com/jriou/covid_adjusted_cfr
The model in the paper is model10, I’m trying some improvements in model11 and model12. I also just added the posterior samples for model10.
Thanks for your efforts. And for your openness.
Sometimes doing nothing is better than putting all the sick and at risk people into “not hospitals”, though.
My understanding is also that it is normal in China to go to the hospital for an IV if you have a cold: https://www.bmj.com/content/348/bmj.g1262
Elsewhere we see only 1-5% of cases are serious or worse, so probably 95%+ of the people rushing the hospital didn’t need to be there. Also, mortality rates were about 4x higher in Hubei vs elsewhere in China (it sounds like there was a coverup of many deaths there so that’s probably an underestimate), so the panic/hysteria was more deadly than the actual illness.
Why were the mortality rates higher in Hubei? I didn’t get the panic / hysteria effect on increasing mortality? Or are you meaning that there was a lot of iatarogenic mortality? Do you mean mortality would have been lower had some people NOT gone to the hospital?
Did you watch the video in my first post? Also go watch the videos from Fang Bin and Chen Quishi before they got arrested.
There’s people everywhere all over the hospitals getting IVs, then they made/built a bunch of “not hospitals” with no doctors or medicine to put people in.
Typo: *Chen Qiushi
In both Italy and Singapore, at least 10% of diagnosed cases have ended up in critical condition in the ICU so far. The reason for the high mortality in Hubei is probably that the hospitals were overwhelmed.
Correct me if Im wrong but in both of those countries aren’t they mostly testing sick people? Ie, that 10% is not 10% of all infections.
I think Singapore has mostly tested symptomatic people, but they have tested quite widely. I’m sure they’re missing some cases, but If there were a lot of undetected infected people, I’d think there would be more random unconnected cases popping up around the island, but that’s not what’s been happening so far. The vast majority of those who’ve tested positive have been connected to one of a few known clusters.
Unlikely. The mortality rate was highest in Hubei before Jan 11, and dropped over time. Poor testing is likely the culprit (both in terms of cryptic transmission, and also in terms of long delays before disease onset and admission to hospital.
This paper is worth looking at. (In particular, Figure 3d)
https://www.dropbox.com/s/v7vylh277uzpse6/Manuscript%20of%20Covid-19%20in%20Wuhan.pdf?dl=0
Thanks.
Arguments from authority are the poorest of all, but we will need to fall back on them as a stop gap, so this about one of the authors looks encouraging https://community.amstat.org/copss/awards/fn-david/2017
This is a very interesting analysis, thanks for sharing it.
> During the outbreak on the ship “Diamond Princess”, nearly all individuals were tested regardless of symptoms, leading to an average proportion of symptomatic infections of 49% in a sample size of 619, which was used in the present study [13]
You may want to update the url in that reference to https://www.niid.go.jp/niid/en/2019-ncov-e/9417-covid-dp-fe-02.html
It currently points to a previous update with only 531 confirmed cases and around 2400 people tested (the latest udpate had around 3000 people tested, out of 3700 people originally onboard).
You use 49% as the proportion of symptomatic infections regardless of age. You assume that older individuals have more severe symptoms and one could naively expect that they also have a larger proportion of symptomatic infections. But the data from which you derive your 49% estimate shows the opposite pattern!
Looking at people aged 20-39, undoubtly most of them part of the crew, we see that out of 775 people there were 52 symptomatic and 10 asymptomatic positives: 84% symptomatic.
Crew members were tested after passengers (and younger passengers were tested after older passengers) so they had more time to show symptoms by the time of the test. One could even make the case that crew members were more exposed and were infected earlier, adding even more time to develop symtoms.
The naive estimate of symtomatic infections is biased low because some of the individuals will go on to develop symptoms later. In this case, we know the bias is larger for older people who were tested first.
Hi Carlos,
Thanks for your input! Yes I realize that the 49% is a weakness of the analysis at this point. The technical thing is that it is difficult to have estimates of symptomatic proportion using RT-PCR and not serology, which is not yet available. RT-PCR tells you whether the virus is present now, serology tells you whether the virus was here at any point. An additional thing is that some of the people without symptoms might show symptoms later as you said. Plus all specificities related to being on a ship: crew members, etc.
On the new version of the model I use another estimate from Shenzen where they found about 80% symptomatics (https://www.medrxiv.org/content/10.1101/2020.03.03.20028423v1).
If the positive asymptomatics later became symptomatic no one has reported on it:
https://old.reddit.com/r/Coronavirus/comments/fem6zv/where_are_the_diamond_princess_passengers_now_has/
How sensitive are the analysis results to the assumption of 49% as the proportion of symptomatic infections? If you change this to 10% or 90%, how do case fatality ratio estimates change?
Better yet, put a beta(2,2) prior on it and do the whole posterior…
Yes this is a weakness I’m trying to fix. A beta(2,2) might be a bit too much in the other direction though!
It will give you samples all over the spectrum, but staying away from 0 and 1. You can then make conditional inferences… if it’s between say 40 and 60 then the results will look like… if it’s between 30 and 40 then… etc.
You might do better to get a more informative prior though. You could also build a sub-model that fits to the available data, princess cruise ship etc.
I would like to help with this effort if you want to email me I would be interested in discussing how to make this model better. In particular I would like to see something like this model able to make predictions about severe cases, and to predict conditional death rates based on the non-availability of care for severe cases after saturating the medical system.
http://www.lakelandappliedsciences.com/contact-us/
Hi Daniel, I just saw this tool for modelling hospital demand. Sounds like it’s in the direction you were interested in, i.e. predictions in the context of medical system capacity:
https://twitter.com/richardneher/status/1236980631789359104
If you p(rior)-hack and redo until you get results you like, is this p(rior)-hacking accounted for in the analysis somehow?
Justin
I understand how priors can be very useful when dealing with something we have a lot of prior info about. But with this infection, there’s not much cumulative knowledge to go around, so all ‘priors’ are wild guesses and change on minute by minute basis.
It is supposed to be accounted for when you check the predictions of a model against new data. You can’t verify your model on the same data used to come up with it.
Another thing to consider is this: https://medium.com/@sesrenaconference/chinas-coronavirus-numbers-are-suspicious-68d4e2b6be6d
Apparently, China reported one million “extra” cases of infectious disease last December.
So this may have started well before usually assumed.
Interesting possibility.
If there was a million cases of coronavirus in December, the virus must be uninfectious indeed if there’s still people on the planet without it.
Or infectious but mild. As long as antibodies dont wane super quickly for some reason I guess that will tell us the answer.
Or perhaps infectious, but mild for many people while very serious for others?
This wouldn’t explain the negative tests coming back in WA.
What do you mean? The data from washington indicates it has been spreading under the radar there since at least mid-Jan:
https://nitter.snopyta.org/trvrb/status/1233970271318503426
Sure, but if there *WERE* 1M cases in China in December and the infectiousness were like we’re seeing, then as Zhou Fang said you’d expect most of the planet would have it by now. identified case load is doubling every ~3 days outside china, in 90 days like that you’d expect 11 billion cases.. obviously it would have slowed but the point is almost everyone would have it already, so you would have almost no negative tests.
What we have is a different situation.
Let’s see what the antibody tests show. This wouldn’t surprise me.
They already had it months ago. The rt-PCR tests are negative once you recover. From what I have seen, I have difficulty understanding how it took so long to spread, and the spread is just happening to coincide with when countries start testing everyone.
Symptoms and disease progression are roughly consistent with SARS, the viruses are very similar. I don’t think that theory that ~ most of the planet already had this disease a month or two ago is anything like consistent with the data available today. For one thing no one I know has had anything more than a sniffle in the last couple months. You might say that sniffle is the virus, but it’s not consistent with the rate of low-symptomatic patients seen on the cruise liners. You’d need something like 99% of the world to be nearly asymptomatic. not consistent.
The current reported case count in WA (Mar 08, 6pm) is 136 about 100 of which are in the Seattle area.
It doesn’t seem to be exploding or doubling every day, but it’s not clear if there’s a problem with testing tools or if that’s been ironed out.
jim, not doubling every day, but doubling every 3 or so outside china overall… There’s TONS of testing problems in WA. You’ll see a big change in the next few days in WA…
Here is the confirmed cases, lower right graph… click the logarithmic version… it’s good enough to a straight line… exponential growth doubling every few days something like 3.
https://gisanddata.maps.arcgis.com/apps/opsdashboard/index.html#/bda7594740fd40299423467b48e9ecf6
No, the idea that a runny/congested nose or sneezing is a symptom of this is false. It is spread by the media leading to people unnecessarily seeking healthcare and causing a panic for no reason.
Absolutely, I agree with you. Anyway, you need way too many asymptomatic patients to make this theory work that we can see doubling every 2 days outside china but at the same time 1 Million patients in China had it in ~ December.
We will see. I think you underestimate the power of the media and authorities adjusting guidelines to create patients out of people who would normally treat themselves at home.
Last Nov I was knocked out for a week w some illness and could barely get out of bed. People in that situation act different when the news keeps talking about a pandemic.
Excellent map, thanks Daniel. Tableau! :)
The map has more reported cases than the state. Also 50 death / > 6000 cases in SKorea? That’s a relatively low mortality rate.
I don’t get silence from leadership! Not just trump, across the board: Fed, state, county, city. Why not just let people know WTF is going on? It’s not about panic. People are trying to make plans for their lives and businesses and need to know whether or not the world is going to shut down. I’ve been telling people here to expect a shutdown for days but county state and Fed all mum.
Jim, my impression is you’re an econ-ish person. If someone “in charge” says “shut down” who gets the blame for the economic loss?
If that same person waits until it’s obvious to everyone that a shutdown is absolutely required, and then thousands die and it seems horrible, and then they mount a heroic effort to help people… Who or what is blamed for the bad thing? and who gets to stand on a podium and look decisive?
hint: first case = the decision maker is blamed for the economic distress, second case = the virus is blamed for the bad stuff, and the decision maker looks good helping the people.
> How do you explain how flu patients have a 19% smoking prevalence?
I wouldn’t explain something that doesn’t exist… rephrase your question to be more precise and perhaps it will become clear to you.
Oops, wrong spot. I’ll try to start a new thread.
Speaking of WA:
The following sounds like a good idea: https://www.npr.org/sections/health-shots/2020/03/08/813501632/seattle-health-care-system-offers-drive-through-coronavirus-testing-for-workers
Maybe you should stop sharing conspiracy theories you saw on Reddit.
If there is data showing China had 1 million more flu cases than normal the month before this virus was announced, that is interesting. Stop trying to shut down discussion of interesting lines of evidence.
You did this with the smoking thing too. It turned out there is not a single publication about SARS or nCoV, including over 1500 patients, that does not show “missing smokers”.
Yes, a lot of what you are posting sounds like some of the fake moon landing stuff.
Conspiracy theories. Rarely the right answer.
So you have fact checked what I’ve posted on this and seen a bad track record?
Please share it. I have been right all along.
“Right all along”?
No, you’re absurdly stubborn in terms of presenting wild claims with very little cherry picked evidence, and demanding ridiculously rigorous evidence to “debunk” claims that aren’t remotely bunked yet. This “one million cases in december” claim is a case in point.
To make a teaching point about this, the common point between the two is basically the failure to construct an adequate null model.
1. For the flu, what do you think is the *natural distribution* of flu cases in China? Do you imagine that infectious disease follows a normal distribution? What do you think is the underlying assumption that your professor of philosophy uses when they look at a december spike in infection disease over three scant years of data and figures this is an unexpected pattern?
2. For smoking, what do you think is the *expected proportions* of smoking status amongst people at a particular hospital in Wuhan? Consider that in the initial stages of the infection only a small proportion (10-20%) of cases were showing up to the hospital – and that therefore a major confounding factor is *how health conscious* the individual is and how that factor motivates them to go get diagnosed. Consider that individual locales like Wuhan can have very different patterns of smoking to the national average. Consider that scared individuals can lie to doctors because they fear that they might be blamed for their infection. Without securing these factors, you simply cannot just compare surveys in totally different contexts.
The smoking thing isn’t limited to Wuhan. It is every study of SARS and SARS two that eve mentioned smoking. But this is not seen for MERS, flu, or any non-infectious diseases checked.
If it’s some problem with the data, somehow that only affects data regarding viruses that target ACE2, they should be figuring that out, not igoring it.
For example someone can publish the rate of male smokers vs male nonsmokers.
And I never claimed those flu cases were the virus, I said they could be. You don’t even want to consider the possibility. I don’t know what your list of strawmen was supposed to show. Either go figure out the distribution or ignore it, don’t dismiss ideas just because you don’t like them and then assume you are right.
https://www.reddit.com/r/COVID19/comments/faluhv/an_exhaustive_lit_search_shows_that_only_585_sars/
A plural of bad analyses doesn’t make for any meaningful evidence.
You have zero evidence it is due to a data problem. All the evidence shows a lack of smokers, but you stick with your dogmatic assumptions, not even wanting it to be investigated further. That is not science.
Sure it could be due to a data problem, but it’s very unlikely for data issue to *only affect viruses that require ACE2 to infect cells* and nothing else.
As more data comes in it has supported that this is real 100% of the time. You are immune to evidence.
Of course who cares about us on this blog, but more importantly I suspect your attitude is shared by many journal editors and health authorities. They really would prefer to let millions die before even allowing consideration that smoking may be protective.
Changes in the lungs of smokers could be protective but there is very little reason to believe short term smoking would be protective, and much reason to believe long term harm would result. Are you seriously suggesting we should try recommending a short term smoking trial as potentially protective? You know what’s protective? Washing your damn hands and not picking your nose. Also avoiding crowded areas. And zero long term harm. The smoking thing is interesting to study the biology and use the info to maybe understand mechanism and design drugs… Not as a short term prevention. There are many lower risk preventatives
> You have zero evidence it is due to a data problem. All the evidence shows a lack of smokers, but you stick with your dogmatic assumptions, not even wanting it to be investigated further. That is not science.
We already have that one study that showed that the effect is due to confounding with “health worker status”. The argument is not that it’s a “data problem”, the argument is that there is no model here, no controls, only a set of assumptions and no attempt to sort out confounders.
> Sure it could be due to a data problem, but it’s very unlikely for data issue to *only affect viruses that require ACE2 to infect cells* and nothing else.
Nothing else? Oh, have you looked at *every virus* to see if there’s a presence of confounding with smoking status?
Look for example at
https://onlinelibrary.wiley.com/doi/pdf/10.1111/j.1467-842X.1999.tb01555.x
They collected smoking status from 191 patients of all sorts of different cases in an Australian hospital in 1991. Of those, 13% reported as smokers. Prevalence of smoking in Australia at the time was >30%. Proof that smoking protects from *everything*?
Or at
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4428849/
Brazilian study. 100% of 104 asthma and COPD individuals in the study declare themselves to be non-smokers. Impressive coming from a city where 20% of people smoke. Does smoking cure asthma and COPD?
Oh wait, when they do the chemical test it turns out 31 patients were lying about their smoking status. Oopsy.
> As more data comes in it has supported that this is real 100% of the time. You are immune to evidence.
>
> Of course who cares about us on this blog, but more importantly I suspect your attitude is shared by many journal editors and health authorities. They really would prefer to let millions die before even allowing consideration that smoking may be protective.
None of the “data” has remotely addressed any of the major issues with your assertions. Instead you double down, claiming a massive global conspiracy to amongst all journal editors and health authorities to kill millions of people. This is nonsense conspiracy theory logic.
To Daniel: actually asthmatics are underrepresented too so I suspect it requires chronic inflammation. The best case is probably having quit rather recently.
However if short term smoking did work that would be a pretty safe and cheap treatment. The point is they need to study this and figure out what is going on instead of ignoring it.
To Zhou Fang:
This is *every single study*, not some random ones you cherry picked. 100%, no exceptions. In fact here’s another one found today: https://www.ncbi.nlm.nih.gov/pubmed/32146694
2/20 “adults” (> 15 years old) with a history of smoking vs 42% expected.
There have been *no exceptions*, totalling over 1500 cases.
“Every single study” can have the same error. In the Brazil study *every smoker lied about their smoking status*. If people in China lie about their smoking status it doesn’t matter how many different samples you take from that population, every one of them is nonsense. The systematic error in your analysis is merely repeated over and over again. Your conclusions are meaningless.
> If people in China lie about their smoking status
This was already addressed. If that is what was going on then we would see this for many studies in China.
Instead we only see it in SARS and SARS2 studies, both viruses that require ACE2 to enter cells. The expression of ACE2 in the respiratory tract has been reported multiple times to be altered by tobacco smoke. Most say it’s downregulated, one paper says expression changed from club cells to goblet cells (ie, higher in the tract).
I noticed your random studies weren’t even from China. According to you the Chinese are often lying about smoking status, it should be easy to find a bunch where smokers are underrepresented from there then (no doubt you can find one or two, of course… But I haven’t even seen that).
And why would they lie about smoking when healthcare is free so it doesn’t affect anything? Further 60% of doctors smoke and its seen as masculine to smoke? There is no incentive to lie there, at least for men.
Your assumption is in conflict with the observations.
> This was already addressed. If that is what was going on then we would see this for many studies in China.
Okay, then present some studies from China where the participants can be proven to not lie about their smoking status. How many studies from China *not* related to SARS have you reviewed? Even a single one?
Here’s a Beijing study of influenza giving only 8% of influenza patients (and 15% of uninfected patients) saying they are current smokers. I suppose it must have slipped your “we only see it in SARS and SARS2 studies” sweep.
https://www.ncbi.nlm.nih.gov/pubmed/28456530
What exactly would it take to show your methodology is silly? How far do people have to go to *disprove* a thing that you haven’t remotely proven?
So funny, look at the data. 40% of the patients are under 5 years old! You need to calculate the rate only for *adults*. And yes I was already aware of this study.
Here is a study of COPD where ~63% of people had smoking history: https://www.ncbi.nlm.nih.gov/pubmed/31330521
Here ~22% of households had at least one smoker: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5304575/
Here 17% of pneumonia patients were current smokers: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4236731/
I’ve got another post in the spambin, but here is one where ~19% of flu patients over 15 years old report being current smokers:
https://bmcinfectdis.biomedcentral.com/articles/10.1186/s12879-019-4181-2/tables/3
You can cherry pick the 7/81 14-59 years old 2011-2017 datapoint I guess if you want.
Here is a 2020 review that collected 10 papers. They found 947/2971 (32%) of people over 60 (the same agegroup overrepresented in nCov-19 data) report smoking:
https://www.ncbi.nlm.nih.gov/pubmed/32115605
31.2% of acute heart failure patients are smokers:
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5581412/
This one is actually pretty low, 21.7% of patients hospitalized with heart failure reported a smoking history: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6755852/
25.6% of hospitalized heart failure patients reported smoking:
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6726881/
But when it comes to SARS and nCoV-19, only 5-10% of patients report smoking.
You use the word cherry pick a lot. The word doesn’t mean what you think it means. The point of all these studies are *the self-reported smoking numbers are different*. The indication is pretty clear that there is not expected to be any consistent connection apart from clinical ones, because self-report of smoking to doctors is clearly a function of a wide range of demographic, geographic, and psychological factors.
> self-report of smoking to doctors is clearly a function of a wide range of demographic, geographic, and psychological factors.
Yet in every case from China smoking is reported *at least* 2x the rate we see for SARS and nCoV-19. You assume that is because Chinese patients do not want to tell their doctors about smoking.
But it seems they only do that when it comes to SARS and nCoV-19. Two virus epidemics separated by about 20 years and requiring ACE2 to infect cells, whose expression is said to be affected by smoking.
Let’s not investigate this at all, you are satisfied with your assumption.
Take those numbers you picked, do a simple z-test. What’s the probability of a particular scenario like coronavirus having a self report rate of <10% by random chance? 0.1391.
The "demographic comparison" methodology is useless.
> Take those numbers you picked, do a simple z-test. What’s the probability of a particular scenario like coronavirus having a self report rate of 15 years old) I’d love to add it.
You have been unable to find a single piece of evidence to support your assumption that the missing smokers are due to underreporting of smoking in China.
If you want to do pointless calculations: What is the chance of observing a sample of 215/1847 (11.5%) smokers when the population frequency is ~25%?
Stray greater than sign last post. Here is he correct one:
> Take those numbers you picked, do a simple z-test. What’s the probability of a particular scenario like coronavirus having a self report rate of <10% by random chance? 0.1391.
I didn't pick any numbers. Those are all the numbers I found. If we add your paper we would have another ~25% smokers in adult flu patients number. If you can find more numbers about rates of reported smoking in china (in adults, > 15 years old) I'd love to add it.
You have been unable to find a single piece of evidence to support your assumption that the missing smokers are due to underreporting of smoking in China.
If you want to do pointless calculations: What is the chance of observing a sample of 215/1847 (11.5%) smokers when the population frequency is ~25%?
Extremely high, **when you are not doing a random sample**. That’s the point.
If the population level is 30% or whatever, but one study finds 17%, one study finds 63%, one study finds 19%, the clear and obvious reality is that when you get a person into a hospital and ask them whether they smoke or not, there’s something very complex going on that is not “well, we randomly pick some guys and know their smoking status”.
You might have a case if every other ‘null’ study showed exactly 30% smokers, but from scenario to scenario, things vary massively, and in ways that cannot be accounted for by a naive random sampling method. You might get excited at 11.5% but 19% already puts 25% outside the confidence interval! If we adopt your methodology, smoking prevents the flu!
One can speculate exactly why this is, but clearly it happens, and because it happens, your method is meaningless.
> You might get excited at 11.5% but 19% already puts 25% outside the confidence interval! If we adopt your methodology, smoking prevents the flu!
This is not even close to my methodology. That may be how *you* look at data, which may explain why you cannot see what is obvious. I would never do NHST, it is total pseudoscience.
Instead I compare how well different explanations explain what I observe. The “dont tell the doctor they smoke” explanation does not explain what we see at all. The “ACE2 is downregulated (or whatever) which makes smokers respiratory tracts less susceptible” explanation works great.
If someone has another one I am glad to consider it, but yours is awful.
How do you explain how flu patients have a 19% smoking prevalence? Why is 11.5% special and 19% not?
There are many legitimate critiques of hypothesis testing, but if you want to go from that to “well I feel fine thinking the observation that my result is the lowest of five numbers is Super Important” regardless of how variable those are and how the variability doesn’t fit at all your model of how these numbers vary, then you’ve fundamentally misunderstood Andrew and this blog.
I don’t even know why you think it’s so incredible people would underreport smoking. Firstly your ‘60% of doctors smoke’ is itself highly variable, with estimates going down to 15%. Secondly not paying still leaves lots of reasons to misreport (not that patients had financial incentives to lie in the Brazil case). Perhaps patients thought that hiding smoking history would force doctors to treat coughs more seriously. Perhaps the definition of smoking differed subjectively, and these patients considered that they smoked, but not seriously. Perhaps these patients are responding to the recent Wuhan government anti-smoking campaigns (http://www.chinadaily.com.cn/a/201807/03/WS5b3b220aa3103349141e06c9.html ) and didn’t want to get into political trouble. Lots and lots of explanations.
It’s clear at this point that talking to you is an utter waste of time. Hopefully someone else finds what I’ve said useful.
Zhou, I appreciate your push-back, I think you bring up important points. I honestly don’t care about the smoking question, but I think the points you bring up are good points in any question of inference.
> don’t even know why you think it’s so incredible people would underreport smoking.
I don’t… I find it incredible this happens every time but never to even close to the same extent for anything besides SARS and nCoV-19.
But you knew that, because I have repeated it half a dozen times now and you tried to find evidence to the contrary and it turned out the best you could find was from a bunch of five year olds.
Anoneuoid and Zhou Fang,
Maybe the larger point here is that it would be useful to have a case-control study of risk factors for COVID-19. I am surprised not to have seen that kind of study yet, but maybe it will show up in the next few days.
I agree the smoking association is likely artifactual — perhaps people don’t report honestly about smoking habits, especially if they are in the middle of coughing (which is… a symptom of covid 19). The reported prevalence of current smoking could also be sensitive to small differences in the definition of smoking. But overall, a risk factor study would be great at this point.
One could compare family members infected by an index case with family members who were not, for example. Risk factor data could even be collected prospectively, after the index case is diagnosed but before any family members show symptoms.
I’d also like to see data on drinking behaviors among patients with covid 19. Some studies find that drinkers have reduced susceptibility to the common cold (which is sometimes also a coronavirus), reporting odds ratios of about 0.2-0.8. For example, see Ouchi et al. 2012 (PMID 23158193) and Cohen et al. 1993 (PMID 8363004). Since smokers are especially likely to be drinkers, this could explain some of the ostensible negative association between smoking and covid 19, though the association between smoking and drinking would have to be extremely strong to explain much of it.
I caution that the idea of a negative association between drinking and covid 19 is a total shot in the dark. Despite mentioning it here I believe it is almost surely wrong! However, given the studies mentioned above, it seems worth asking participants in risk factor studies about amount and frequency of drinking, if only to cross that very small possibility off the list of relevant risk factors.
Thank you. The more data the better on this.
New paper reports 11/191 patients are current smokers: https://www.thelancet.com/lancet/article/s0140-6736(20)30566-3
No data on drinking.
May have model implications, children may be asymptomatic carriers that show little to no symptoms, instead of just not catching Coronavirus:
See: https://www.nature.com/articles/d41586-020-00154-w
“This may be the first clear evidence that children are as susceptible as adults to SARS-CoV-2 infection,” says Ben Cowling, an infectious-disease epidemiologist at the University of Hong Kong. He now wonders whether the fact that outbreaks haven’t been observed in schools could be down to the fact that children’s symptoms are mild.
Lessler says it’s still not clear whether children are important in transmitting the virus, as they are with influenza, where children routinely develop symptoms and are common hubs in chains of transmission. “That’s one of the current critical remaining questions and we’re trying to figure out how to answer,” he says. “I have a 7-month-old and a 6-year-old and I can’t imagine that, if they have any virus at all, they’re not getting it on somebody.”
The study could have important implications for slowing the spread of the virus through measures such as school closures. “Once we say containment is not an option, we can’t ignore the kids,” says Lessler.”
+1 school closures most likely need to happen today in densely populated areas like LA county or NYC or Atlanta or Boston or whatever.
The concern is that with cases doubling every ~ 3 days at the moment… things will be 1024x worse first week of April. Unless we do something NOW to slow the spread, you’d expect maybe 500k confirmed cases in the US by first week of April and maybe 50k of them need ICU based on Italian estimates, that’s 50% of the ICU capacity of the country… 3 days later you’d need 100% of the ICU capacity… 3 days after that 50k people will show up for ICU and zero of them will get sufficient treatment. Case fatality rate will spike at that moment and stay very high, maybe around 10% until the active severe cases drops dramatically below 100k again and everyone can have an ICU bed (and this isn’t even taking into account how many healthcare workers will be sick reducing ICU ability)…
We need to slow the spread dramatically starting NOW so that first week of april we are still standing up. As someone who was sick continuously for about 5 years after my kids were born, I can’t believe that closing preschools and K-12 schools would hurt this effort, even if it isn’t for the purposes of protecting the children directly, just keeping their parents and especially grandparents out of the ICU is reason enough.
I don’t know about the US but I do have some knowledge about the UK response to Coronavirus. Quite a lot of work has previously been done modelling the response to a pandemic (of influenza, but it applies to any virus).
Closing schools is disruptive, and for how long do you close them? Will closing schools have any substantial effect on spread? The answer to these questions is not as obvious as you seem to believe. The socio-economic disruption due to a disproportionate response may be greater than that of the disease itself.
It may be, but when uncertainty is high, rational decisions are dominated by the tail. SARS had 55% case fatality rate for people over age 65. In the 1918 pandemic flu worldwide, the case fatality rate for over 65 was ~ 1.5%
Case fatality rate is estimated above at on the order of around 10% to 36% for over 65 and still up in the 1% range for middle aged, 40 ~ 60 year olds.
1918 flu killed between 20 and 100M people worldwide, hard to estimate exactly. We could do exactly nothing, in which case from comparisons between the two and change in total population, and particularly the extremely high rate among the elderly, you might expect ~ 200M to 1 billion people dead by next year? To avoid that cost, how long should we simply all stop doing anything but providing food and medical attention? Certainly well over 12 months. Obviously some intermediate between near total shutdown for 12 months and do nothing is the optimum. But it’s far from “do nothing”.
I’m interested in how things would change if any of the many priors and hyperparameters would change. Was there any sensitivity analysis done?
Also, is there any dichotomania/categories are bad/whatever the critique against frequentism is today/etc. issue here by discretizing age? Seems like there could be, 59.5 vs 60 years old, for example.
Justin
Justin:
This sounds like you’re trolling. If you want to troll, I recommend you go over to Marginal Revolution: they have tons of interesting blog posts and an active, vibrant trolling community in the comments section, much more fun than trolling here, I’m sure.
But to take your question seriously: Sure, you can increase the number of age categories and see what happens. Sometimes when we add categories we need more regularization to handle the additional parameters. As noted in the above post, all the data and code are publicly available, so if you have thoughts on how to improve the model by in any way, go for it.
+1
Andrew:
Aren’t you overreacting?
How is this any different from the “blood sport” guys. These sound like questions, no more provocative than what someone like Aneuneoud regularly posts on the blog.
Rahul:
I have no problem with vigorous debate and solid disagreement. The reason this looks like trolling to me is not that it’s provocative, but that I don’t see these as sincere questions. We have an excellent comment section, and I don’t want it to get filled up by people who are just tossing off insincere comments.
But it’s very difficult to discern intonation from typed speech, so I did give the question a straight answer.
Having read Justin’s blog, I’d say he’s a radical frequentist rather than a troll – a different beast even if just as loathsome.
(The comments section of MR is horrible, don’t send him there!)
This is for deaths. Has anyone done a similar analysis for serious cases? I’d like to know my likelihood of needing an ICU or being at risk for lung damage if infected.
+1
+1 especially since one of the primary risks seems to be a collapse of the healthcare system. Is this just a much more difficult quantity to estimate?
“Is this just a much more difficult quantity to estimate?”
I would guess so. I doubt there is much date on past instances of a healthcare system collapsing, so would guess it would be a matter of speculating on contributing factors and which ones are most important — with lots of conflicting opinions.
I don’t understand what is being used for treatment. If one is infected with a virus the knee-jerk reaction is that antibiotics will not help cure the illness. But, as we know, respiratory viral infections like influenza are often followed by very dangerous bacterial secondary infections that cause a lot of damage to lungs by virtue of feeding on the debris from the destroyed lung cells. There are no comments that I can find about the treatment methodologies if any, employed for the seriously infected folks. Obvious comparisons of various treatments will have a large impact on the death rates observed. If the viral infection continues for 14 or more days, bacterial pneumonia will take over.
https://www.ncbi.nlm.nih.gov/pubmed/18710327
J Infect Dis. 2008 Oct 1;198(7):962-70. doi: 10.1086/591708.
Predominant role of bacterial pneumonia as a cause of death in pandemic influenza: implications for pandemic influenza preparedness.
Morens DM1, Taubenberger JK, Fauci AS.
Good point. Does anyone have information on deaths from COVID19? In particular, is the virus itself the direct cause of death, or is an opportunist infection such as pneumonia the cause of death? Or other possibilities? (e.g., fatal reaction to medication or. the aspect of treatment?)
The deaths are mostly due to ARDS.
Anoneuoid, Prior to the development of full-on ARDS (Acute respiratory distress syndrome ), there has to be an underlying cause of the syndrome, of course. Is it the virus, or is it the secondary bacterial infections? If it is the latter, then this can be treated with antibiotics and these may ameliorate the process prior to ARDS, thus saving lives, even though the virus may not be impacted by this treatment.
“What
Really Happened during the 1918 Influenza Pandemic? The Importance of Bacterial Secondary Infections
John F. Brundage, G. Dennis Shankshttps://pubmed.ncbi.nlm.nih.gov/18008258-what-really-happened-during-the-1918-influenza-pandemic-the-importance-of-bacterial-secondary-infections/
https://academic.oup.com/jid/article/196/11/1717/886065
If that were the issue I believe it would be better than the actual situation. My understanding is that in Wuhan at least death often occurs around day 10 to 20, whereas symptoms start around day 5. I don’t think it’s enough time that bacterial secondary infections are the cause.
I believe that there is some evidence that cytokine storms leading to enormous immune response in the lungs tears that tissue up, and people essentially destroy their own lungs… SO perhaps significant steroid treatment would help. You’ll have to do some googling for info on that, my wife mentioned some links but I don’t have them to hand.
Please see my post below about aspirating the excess mucus. For some reason recently my posts keep showing up in the wrong place on mobile if I switch tabs, sorry.
Oops — should be “other aspects of” rather than ” or. the aspect of”.
A possible factor in the mortality associated with COVID-19 at this time is that the pneumonias that follow are generally not bacterial pneumonias and thus not treatable by antibiotics, unlike the usual pneumonia-after-flu. Check out https://www.thelancet.com/journals/laninf/article/PIIS1473-3099(20)30086-4/fulltext for some initial discussion (“Radiological findings from 81 patients with COVID-19 pneumonia in Wuhan, China: a descriptive study” from the Lancet Infectious disease mag online)
Below is a copy of an email sent out today to faculty by the provost of my university. I am wondering if this is a
typical response to COVID-19 concerns, or if there is wide variation in how colleges and universities are responding?
Dear faculty colleagues,
We recognize the emerging COVID-19 (coronavirus) public health concern is creating a great deal of uncertainty for our campus community. As this global situation evolves, our goals remain the same — to take care of our community members in need and to ensure minimal disruption to our educational mission through contingency planning.
As spring break approaches, we encourage you to consider how travel plans could be affected by the spread of the virus and urge you not to travel to countries that have been designated as CDC Level 2 and 3. Please take precautions and monitor the UT Restricted Regions list if you are going to travel internationally.
We are currently developing plans to maintain the continuity of the educational experience for students and faculty members who, for reasons related to COVID-19, will not be able to return to campus. This includes students returning from study abroad in regions of concern who will be in self-isolation.
During this challenging time, we ask you to be supportive of our students. Throughout our university’s history, faculty members have demonstrated great understanding and compassion for our students during times of need, and I thank you for continuing to support them now.
I am writing today to share guidance on accommodations that faculty members can make to support students and to manage teaching needs in the coming weeks.
Academic Accommodation Process
Given current guidance from the CDC to avoid medical offices, faculty members should provide academic accommodations to students requesting them without requiring “doctor’s note” documentation for COVID-19 concerns. I realize this is typically a judgment faculty members are empowered to make, but under these extraordinary circumstances, we are requiring faculty to work with students to make a reasonable accommodation.
To receive an academic accommodation for issues related to COVID-19, students have been asked to submit a request through Student Emergency Services. Students have been provided instructions about how to make this request, but if students contact you, please remind them to do so. After students have submitted the request, faculty members will receive a notification with the names and information of their students who have requested accommodation.
This process applies to ALL students — undergraduate, graduate, doctoral, professional and law students.
Types of Academic Accommodation
Faculty members have broad discretion to make accommodations for students in response to the COVID-19 situation. Although faculty members cannot alter the grading policy for their courses, they can make accommodations for demonstration of engagement/participation or alter the weighting of assignments to account for a students’ circumstances.
Other examples of faculty accommodations for students who are sick or in self-isolation due to COVID-19 concerns include, but are not limited to:
Creating online options for students to participate remotely. This can be done through ZOOM or other platforms provisioned by your college or school. Learn more about alternative methods to continue instruction.
Providing online office hours via Canvas, email or phone. You can also allow for course discussions and class contributions via Canvas.
Assigning a note taker to share information with students who are not able to attend in person. This person can post notes on Canvas or through other online channels.
Extending deadlines for assignments, if possible.
Creating a curve to adjust for reduced performance by the class relative to historical norms.
Give special consideration for students in their final semester who intend to graduate in May and whose class performance may have been impacted by COVID-19 issues. Their grades this semester will determine whether they meet requirements for graduation. Before assigning a non-passing grade to a student who is affected by COVID-19 and intends to graduate, please work with the student to ensure he or she has the opportunity to complete the course.
Scheduling remote thesis/dissertation meetings for graduate students who are sick or in self-isolation.
Reminding graduate students they can submit their final paperwork required for graduation by mail. Most students visit their office for this purpose and may not be aware of the mail option.
Sick & Self-isolating Faculty
If a faculty member is ill due to COVID-19 concerns, unable to work or is working part time due to illness, then he or she should use sick leave for the hours of work that are missed. Faculty members who self-isolate are encouraged to communicate with their unit’s (department’s or college/school’s) HR contact to ensure coverage for missed classes and meetings. If a faculty member’s department (or host unit) becomes aware of a possible need for Family Medical Leave, he or she should notify HR, which will send relevant information to the faculty member. Information summarizing sick leave and related policies for faculty members can be found here.
If a faculty member self-isolates due to possible exposure to the COVID-19 illness (although the faculty member is not symptomatic and is able to work), he or she should endeavor to teach and meet with students and colleagues remotely. Faculty members are encouraged to immediately consult with their department, program chair or the Dean’s Office to identify relevant resources, expectations and information for working remotely. Faculty members should also immediately notify supervisors, students, staff members and faculty members of their plans to work remotely, as well as their plans for covering missed class sessions, office hours and meetings.
Continuity of Classes Through Online Options
Although at this time the threat of COVID-19 does not necessitate a widespread transition to online classwork at UT, we are taking steps to ensure the campus is prepared in the event we need to do so. If we do reach that juncture, you can expect information and direction on how to implement the necessary changes. Faculty members should not transition to online classwork without first receiving direction from the UT administration.
The Faculty Innovation Center has information and guidance about teaching remotely using technologies such as Canvas and ZOOM. ZOOM can be used to host meetings with multiple participants and is able to record class and meeting conversations.
International Travel Booking — Policy Update
Effective March 6, 2020, all international university-related travel must be booked by the UT Austin contracted travel agents or Concur UT’s online booking tool.
Given the evolving situation with COVID-19 (coronavirus) and in an effort to protect employees’ health and financial interests, travel to CDC Level 2 and 3 travel advisory locations for coronavirus is restricted. Travel to these areas will require authorization from the International Oversight Committee as well as additional university authorities. Travelers will be required to forward their International Oversight Committee approval letter to the travel agencies prior to airfare issuance.
Information about business travel-related reimbursements for trips canceled or postponed will be shared when those details are available.
Expect Additional Guidance – Give Feedback
We will continue to share more guidance and information with faculty members and the campus community as the circumstances evolve. If there are topics you feel are not being addressed, please share them with us at [email protected].
I want to continue to stress the importance of regular hand-washing and other preventive measures. And if you are feeling ill, it is important to stay home from class, events and your workplace. Preventive actions you should take include:
Wash your hands often with soap and water for at least 20 seconds.
Keep your hands away from your nose, mouth and eyes.
Cough or sneeze into your elbow.
Use verbal forms of greeting in lieu of handshaking.
Thank you for all you are doing for our students and for one another during this challenging time. You can expect more information as it becomes available.
Coronavirus Updates and FAQs
utexas.edu/coronavirus
Yes, this is typical I think. My wife says USC is specifically dedicating next week to testing online teaching with students and faculty through ZOOM, the following week will be spring break. Her colleague who is isolating due to exposure to Italy at a conference expects that classes will be entirely online when things resume the week of the 23rd.
I think this is all great. Honestly the technology is good enough these days that online classes are probably *better* in many cases anyway, so cost is minimal if not in fact a benefit. The reduction in exposure is helpful.
It depends on the class. Moving lectures online works OK, but labs or discussion-based seminars are not so easy to conduct online.
True, short term labs will be disrupted for millions of people for weeks and weeks, long term hundreds of millions of people will be forced to adopt beneficial technology whose benefit continues to accrue forever.
So everyone got forced off skype by now? Microsoft really destroyed that useful tool, it became unusable for me about a 2 years ago and I switched to zoom.
University of Washington closed classrooms last week. All classes are now via web.
Miguel has some informative tweets https://twitter.com/_MiguelHernan that might be helpful and this one in particular #flattenthecurve (the advantages of slowing down transmission).
Miguel Hernán: “If we’re going to close schools eventually sooner is better”
Thank you, finally
Further discussion of the “dark smokers” should go down here.
The rate of smoking in cases of the flu in China is 42.5%, not 19% as Zhang claimed above:
https://www.ncbi.nlm.nih.gov/pubmed/23958687
Yes, I am being sarcastic but maybe it will make sense to them.
So this is interesting primarily in an end-game scenario where essentially 100% of people are infected. It tells us we’ll “only” see 21 million dead by say… december as opposed to if it really is say 1.5 or 2% and we’ll see 105M dead by december…
Of course, if it goes like that, the healthcare system will be completely overwhelmed, and case fatality rates will skyrocket when ICU and respiratory help can’t save people… so all bets are off as to how helpful any of that is… if everyone gets it and 10% need ICU to survive and ~ none of them get it… then we’ll see 700M dead by December.
A more realistic scenario is truly severe isolation once everyone super-panics, clamping the virus to ~10% infected worldwide, and somewhere between say 0.3% and 10% dead depending on ICU needs etc… so that’s 2.1M to 70M dead by december.
The “best case” is that organizations who have been preparing for this sort of thing attach their balls and tell the president and pence and other leaders to fuck off and quit their job and then get a permanent mouthpiece in the NYT and LA Times and London and soforth… saying “here is what you do… get into hideout mode… stop the spread… it works” hopefully in the next ~ 15 days, and then maybe we wind up with “only” 5-20M cases worldwide or some such number and death rates really are around say 1% because ICU and health care can cope, and then we have something like 200,000 dead like in a severe flu year.
So those are the options roughly, back of the envelope… which one do you want to do? I can tell you that my kids are not in school and I have food for several weeks at my house. Cost of that plan is minimal compared to the alternative.
I’m not the only one doing these kinds of numbers, this is a typical engineer thing to do, you want to know how many tons of steel you can get moved from place to place by a certain date… or whatever, so you run some scenarios… and the scenarios this bio-engineer runs look a lot like mine:
https://threadreaderapp.com/thread/1236095180459003909.html
Back in the middle of Jan I would have agreed with you. That was the time to shut down travel, etc. Now it is far too late, and the infection and mortality numbers are primarily measuring the number of tests.
is the large increase in intensive care patients also a consequence of the number of tests performed? Let’s stop testing, then, and no one will die!
I mentioned it above that I was knocked out by some illness in early November last year. I literally didn’t leave my bed except for the bathroom for a week. And even that was difficult.
If I was over 50 and heard constant coronavirus chatter going around I could easily see that I ended up in the hospital and then ICU instead of just dealing with it.
Maybe someone that decides who gets in the ICU can correct me.
If you are over 80 and contract pneumonia you don’t get an ICU bed (because it’s futile).
This was true pre-Coronavirus. Pragmatically, you get oxygen and comfort care, and you make it or you don’t.
At the moment in Italy it’s reported the cutoff is now 65, or if you have any comorbidities regardless of age. Italys lockdown will be effective but there are already 10 days of lag… so over the next 10 days it will grow, and the criteria for an ICu bed will be someone on ICU just died, you are under 50, and you rolled a 1 on a 6 sided die
Aargh!
I don’t know those details. I do know I read they started aspirating mucus in China and claimed it cut mortality of the ARDS patients in half, but for some reason this is hard to find. Liu Liang was the main guys name iirc.
I would like to know how many cases of coronovirus are connected to vape use. Vape is a liquid taken directly into the lungs. It’s volatile, severe allergic reactions.
w. r. t outside reference points, we have data on small islands eg. st. barth, pop c. 7000, daily average contacts 600 (550 tourists + estimate for sundry people.
On the technical side, I had some ideas. Wonder if they made sense and if any of these tools (apps) already exist:
One of the big tools in the response is transmission tracking and isolation. Going ahead this seems a common part of the response to any pandemic.
But from reading the news this seems to be still done in a relatively primitive way. These days most everyone has a smartphone. With a combination of GPS and perhaps blue tooth shouldn’t it be possible to create a list of potential contacts? This way, the moment a positive for an infection is detected (through a symptomatic case, or random screening etc.) instantaneously a list of probables for infection transmission could be generated and then triaged. Not sure how much damage reduction we already can do but surely for future pandemics this sort of thing can squelch the spread right at the start?
Perhaps, GPS alone will generate a moving circle too large for this to make good use of; typical transmission tracking would want to only target other users in say a 4 to 6 feet radius. But assuming we turn on things like Blutooth, or even better NFC or maybe even out-of-hearing bandwidth sound pulses (e.g. how the google stick uses for pairing) etc. couldn’t this be made more refined for short radii interactions? Other tweaks could be some sort of time integral of proximity to come up with probabilistic estimates of who could have been infected. Finally, I can even imagine doing more fancy stuff like estimate who used the same hotel room the next day or who sat in the same taxi cab etc. Using known databases of WiFi router names (thanks Google!) or Cellular IDs or things like Foursquare I suppose one could further refine such a tool?
Of course, this raises serious privacy implications and I see several options: (a) A strictly voluntary or opt-in app or feature on the popular phone OSs. I can see many people adopting it out of a sheer sense of doing what is good and right. This way post pandemic people can turn this off as well
(b) Some sort of smart way of integrating this into the OS where the close-contacts-data is gathered by the phone system and integrated only on demand where a certain decryption key is available. Of course, the master key concept has weaknesses so could this sort of thing be made on a voting model where during a pandemic when X% of users vote for it the decryption key is assembled. Sounds like some sort of cryptographic algorithm based on quorum sensing is needed. Not sure if realistic. But basically you don’t have to trust the government to use the tool only when needed but just trust some fraction of the user population.
(c ) Just to suppress privacy concerns right now since these are extraordinary times and in the interest of the greater good.
Fortunately, it does not have to cover the entire user-base. Even with relatively modest penetration one could ease epidemiological tracking efforts or make a dent into the transmission network. Furthermore the most likely spreaders, (e.g. globetrotters etc.) are the ones most likely to have smartphones all the time.
Is anything like this out there? If not, is this sort of tech intervention likely to be useful or a solution in search of a problem?
Rahul I did read somewhere about china implementing some kind of GPS tracking of phones but I think it’s generally something they can do with their authoritarian govt more than could be done in the US.
This kind of surveillance could be important after the initial pandemic flood, in several months, as secondary outbreaks begin to occur and need to be squashed.
I must agree with Jeff Shaman on the case fatality rate. There are two key factors as I see it. One the selection bias on test. Predominantly, People tested are people that have come onto the radar of health services and in these cases the rate of infection must be higher. Secondly the testing for CORVID-19 especially is per my knowledge as to date not yet validated / peer reviewed. It was rushed into use, due to the threatening pandemic. We still don’t know exactly what it finds. (https://www.ncbi.nlm.nih.gov/pubmed/32133832). Based on these factors 2 factors and the fact that overall death rates for europa have not as much as blipped, https://www.euromomo.eu/slices/map_2017_2020.html, I think further research needs to be done to validate testing and models adjusted to allow for accurate representation of selection bias. Further, German data from the Robert-Koch Institut shows no increase in acute respiratory infection in Germany for week 11 2020, https://influenza.rki.de. A good summary of model failures is here: https://www.statnews.com/2020/03/17/a-fiasco-in-the-making-as-the-coronavirus-pandemic-takes-hold-we-are-making-decisions-without-reliable-data
Re-do the age distribution in a pie graph and circulate the heck out of it. This may help the public and the press see that we need to be using a rifle instead of a shotgun for who is restricted from working and being active in the world.
I believe that a random sample study to determine the rate of infection by the virus is fundamental at this stage. The study is purely for determining the rate of infection in the population. The sample size could be determined from standard procedures for random sampling. The sample population is the population of the US. The sample groups are random sample distribution of biometrics of the study. This study should not be expanded for any other purpose than determining the spread of infection rate in the population.
The distribution of all variables of interest should not dictate the scope or methodology for this random sample. The stratification of the results are based on the nature of a truly random sample. This study should be a source of real data collected randomly.
The majority of Americans know enough not to believe the President and /or any of his appointees. Because of this information that the CDC puts out is often deemed untrustworthy. As you all are the experts, would it be possible to distill your findings into an article or summary understandable enough for laymen to consume? Please. People are scared and don’t know who to trust.
I can help connect this model to Facebook data for anonymously and privately tracking phones. Send me email.
How sensitive are the analysis results to the assumption of 49% as the proportion of symptomatic infections? If you change this to 10% or 90%, how do case fatality ratio estimates change?